Johns Hopkins All Children’s opens first-of-a-kind unit for babies with CDH birth defect
In just three years, Johns Hopkins All Children’s Hospital has tripled the number of babies it treats born with congenital diaphragmatic hernia – a hole in their diaphragm, a life-threatening birth defect.
The St. Petersburg pediatric hospital treated 50 children with congenital diaphragmatic hernia in the third year of its CDH program, up from 16 to 18 patients treated in the first year, said Dr. David Kays, medical director of the program.
About half the patients are from families in Florida, and about half travel from around the United States to St. Petersburg for treatment.

Dr. David Kays, medical director, Johns Hopkins All Children’s Hospital CDH program
Now, the hospital has a dedicated Center for Congenital Diaphragmatic Hernia, a 15-bed unit that is believed to be the nation’s first inpatient unit dedicated to the treatment of infants and children with condition, said Thomas Kmetz, president of Johns Hopkins All Children’s Hospital.
The center is staffed by an interdisciplinary team and led by Kays, who was recruited to All Children’s in early 2016 from University of Florida. At UF, he treated 321 children over 23 years – about 15 children a year, Kays said at a dedication ceremony Thursday for the new center at All Children’s.
“I came here to build what I thought would be the world’s best program in congenital diaphragmatic hernia,” Kays said. “There was a trajectory to this children’s hospital that was perfect for this program. I couldn’t take this program to Boston Children’s or Children’s Hospital in Philadelphia. There were too many egos to accept me to come in and change the paradigm. But this place was just right. It had the same vision to be a great children’s hospital the way I wanted to build a great program.”
Continuum of care
About one in 3,000 pregnancies involves a child with CDH, which allows organs such as the intestines, stomach and liver to move into an infant’s chest cavity, threatening lung development. Many women have been advised to terminate their pregnancy when the condition is diagnosed before birth, usually around the 20-week ultrasound.
Surgical repair immediately after birth allows the lungs to grow and mature. Nationwide, the survival rate is 65 percent to 70 percent. At All Children’s the survival rates are over 90 percent, Kays said.
But treatment involves more than surgery, he said.
“People don’t come here for an operation. They come for the whole continuum of care, the whole concept from beginning to end,” Kays said. “The challenge is to keep babies alive who have critically small lungs and that requires a great team of people to have tremendous continuity of care.”
In addition to surgery and in-patient treatment, parents are taught to care for their children once they leave the hospital and return home, said Dr. Jennifer Arnold, a neonatologist and medical director of the hospital’s simulation center. The parents are put through a series of four emergency scenarios, so they can figure out the nature of a potential problem, how to manage it and when to call 911 if needed.
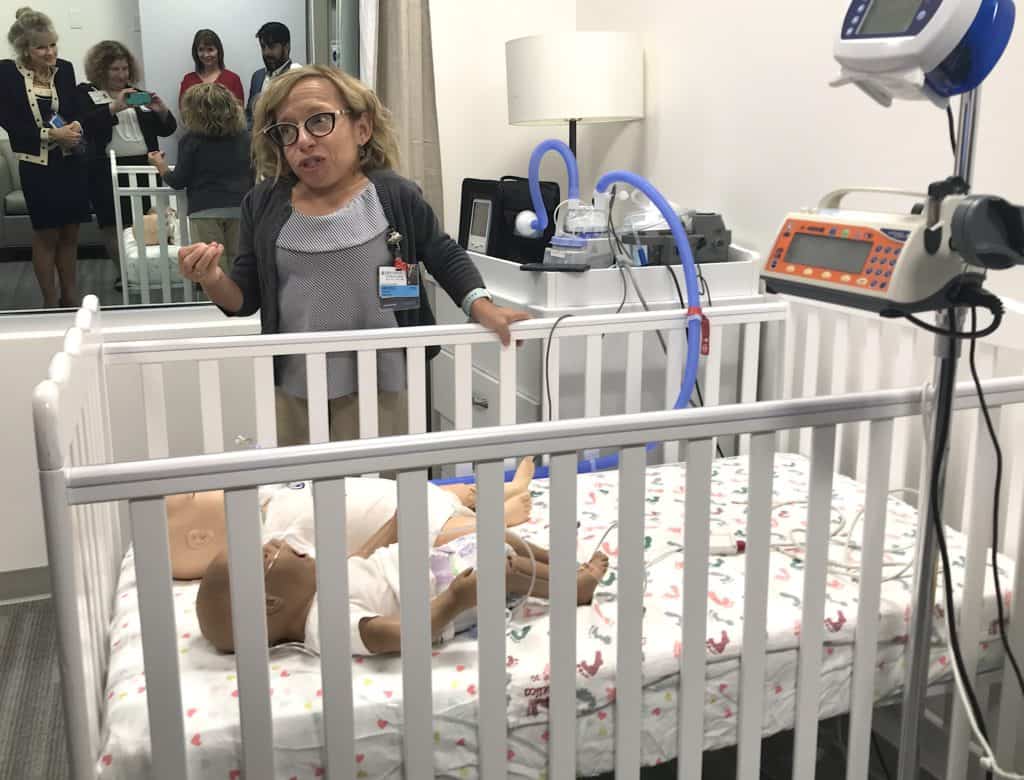
Dr. Jennifer Arnold, medical director, Johns Hopkins All Children’s Hospital simulation center
Dream job

Dr. Stacey Stone, neonatologist, Johns Hopkins All Children’s Hospital
All Children’s CDH outcomes are truly better than anywhere else in the world, said Dr. Stacey Stone, a neonatologist who works in the CDH unit.
“Our babies are not just going home surviving, but they are going home well,” Stone said.
Joy Perkins has worked with Kays for many years, starting at UF, and she is is coordinator for the program at All Children’s.

Dr. Paul Danielson, interim chair, department of surgery, Johns Hopkins All Children’s Hospital
“Being able to bring all of that here and build the program we always wanted to build has been amazing,” Perkins said. “This is dream job. We take care of families every day that are told their children are going to die, and we send them home, and they are doing fantastic.”
Kays has a reputation in the pediatric surgical world as a bit of a renegade, “a hard-driving guy with outcomes so great that some people don’t even believe it,” said Dr. Paul Danielson, interim chair of the hospital’s department of surgery.
Danielson describes Kays as a revolutionary, and the CDH unit as truly interdisciplinary.
“It’s not multi-disciplinary, where different specialties come and work together. It’s where different disciplines come together and create their own new discipline,” Danielson said




Stephen Pirris
November 3, 2019at11:19 am
We are eternally grateful to Dr. Kays, Joy Perkins and their team for our overachieving 6 year old. Most of their children don’t just survive, but they thrive and lead normal lives. Highly recommended for any parents who are facing this devastating diagnosis.
Alison Fisher
October 29, 2019at2:50 pm
We love this team and are forever grateful to them for saving our little boy!